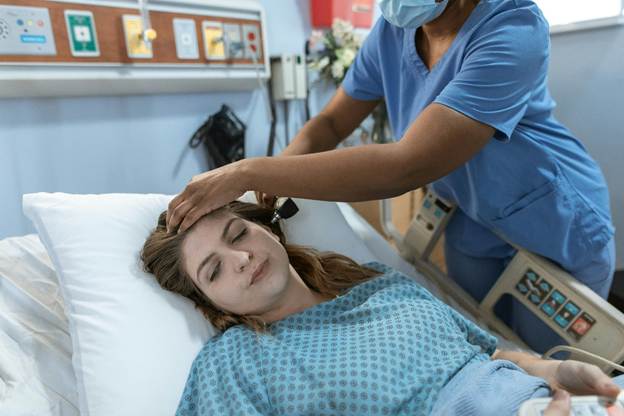
Have you ever watched a patient get passed from one provider to another and wondered why no one seems to fully own the situation? It happens in clinics, hospitals, and even routine appointments, and it leaves people frustrated, tired, and unsure who is actually listening.
After years of working around healthcare settings, you start to notice patterns like this. Not dramatic failures, just small gaps. Missed details. Rushed explanations. Decisions that technically follow protocol but don’t quite fit the person sitting in the chair. Most of the time, those gaps trace back to training—what someone was taught, and what they were never given time or support to learn.
Patient-Centered Care Starts with Judgment, Not Checklists
Patient-centered care gets talked about a lot, but in real settings, it has less to do with kind words and more to do with judgment. It shows up when a patient agrees too quickly, or when a treatment plan makes sense on paper but not in real life. Specialized training is where that judgment develops. Not just learning facts, but learning when to slow down, when to question what looks fine, and when to adjust quietly. Those skills don’t come by accident. Without that depth, care turns procedural. Tasks get done, boxes get checked, and the person slowly fades into the background.
Advanced Clinical Responsibility and Decision-Making
In many healthcare settings, nurses are professionals who operate in the space between standard protocols and complex human needs. They manage long-term conditions, adjust treatment plans, and often act as the steady point of contact for patients who are tired of repeating their story. Their training goes beyond performing tasks. It emphasizes clinical reasoning, accountability, and understanding how medical decisions ripple into daily life.
This is where the advanced nurse practitioner steps in. Advanced nurse practitioner roles and responsibilities include taking detailed histories, adjusting medications, coordinating care with other clinicians, and guiding families through hard choices. These duties aren’t pulled from thin air; they grow from deeper clinical education and hands-on experience.
This kind of preparation matters because patient-centered care depends on continuity and trust. When a provider understands both the clinical picture and the person living with it, decisions tend to be more realistic. Care becomes less reactive. Problems are addressed earlier, often before they turn into something harder to manage.
Training Changes How Professionals Listen
One quiet shift that comes with specialized training is how people listen. Early-career clinicians often listen for the “right answer.” They are scanning for symptoms that match what they were taught. With experience and deeper education, listening becomes wider. You start hearing what is not being said.
This matters more than it sounds like it should. Patients do not always lead with the real problem. They might talk about pain when the issue is fear. Or compliance when the real barrier is money, time, or exhaustion. Specialized training does not make someone magically empathetic, but it gives them tools to slow down and ask better questions, even on a busy day.
Over time, this changes the tone of care. Appointments feel less transactional. Patients tend to share more, not because they are prompted, but because they sense there is room to do so.
Systems Reward Speed, But Patients Need Depth
Healthcare systems tend to reward speed. Short visits, high volume, tidy metrics. Depth can feel like it gets in the way, especially when time is tight. But skipping it has a cost. Confusion builds. Patients come back. Medications get misused. Plans fall apart because they never fit real life. When providers are trained to handle complexity early, fewer problems show up later. It may not look efficient in the moment, but it usually is. Speed fixes today. Training fixes what shows up next.
Technology Cannot Replace Trained Judgment
There is a lot of faith being placed in technology right now. Decision-support tools, remote monitoring, automated reminders. These tools can help, but they do not replace judgment. They surface data. They do not interpret context.
Specialized training teaches how to weigh information that does not fit neatly into an algorithm. A patient who technically meets all the criteria but still feels wrong. A plan that looks optimal but ignores cultural or social realities. These are not edge cases. They are everyday care.
When technology is paired with well-trained professionals, it works better. When it is used as a substitute for training, gaps widen quickly.
Patients Notice the Difference, Even If They Cannot Name It
Most patients can’t name credentials or scopes of practice, but they feel the difference right away. They notice when their story is remembered, when explanations aren’t rushed, when choices feel shared. Trust grows in those small, steady moments. Specialized training helps providers handle uncertainty with confidence, so care stays flexible instead of snapping back to rigid rules when things get unclear.
Patients today show up informed, skeptical, and often overwhelmed, carrying printouts, mixed advice, and very little time. Meanwhile, care itself has grown messier. Chronic illness overlaps. Mental health spills into physical symptoms. Life stress walks straight into the exam room. In that kind of setting, patient-centered care can’t be added on later. It has to be built through training and expanded with responsibility. When that match is right, care feels steadier, with fewer gaps and less confusion about who’s really guiding it.










Leave a Reply